Our services
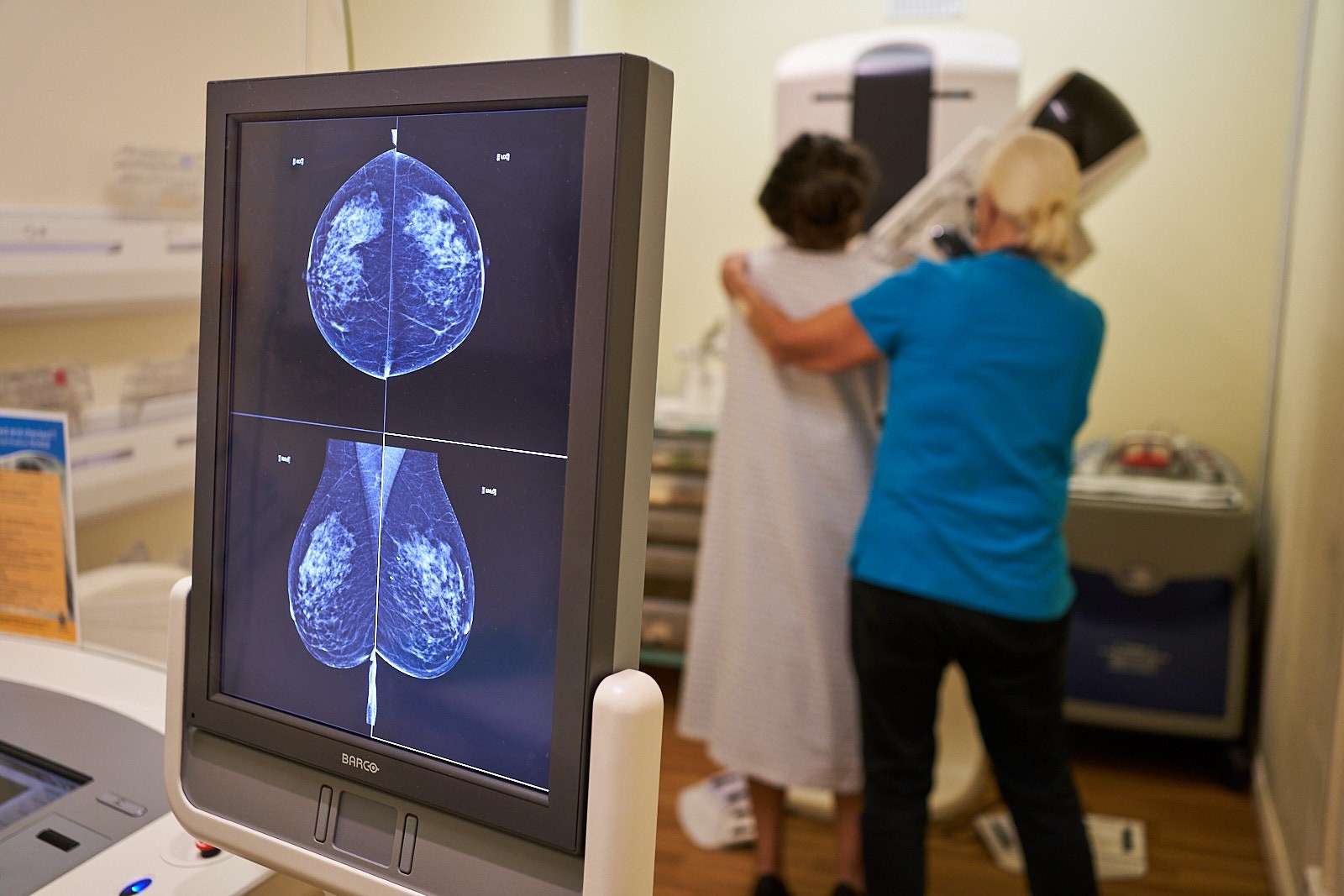
- Breast Screening
- Breast Care Advice
- Breast Cancer Care
- Genetic Testing
- Second Opinions
- Breast Implant Review
- Breast Reconstruction
- Non-Cancerous Conditions
- Other Services
About the clinic
We provide a full range of integrated breast care services for both benign and malignant disease, including screening, surgery, radiotherapy, chemotherapy, reconstruction and aftercare.
Our team, led by specialist breast consultants along with our breast care nurses are dedicated to minimise your anxiety and are available to support you in every aspect of your treatment.
Patient information
Book an appointment
You can call, email or complete a form to book your appointment. We are always happy to help.
FAQs
We have prepared a list of questions and answers to help you on your journey with us.
Fees & Payment
Here you will find information about costs related to our services. This helps us be more transparent to you.